Being a good doctor means to listen, understand and respect the patient therefore sometimes to advise patient to take educated risk to help the patient.
While I was organising the x-rays for this text and thinking what to write, how to explain all the decision taking and reasoning behind the decisions, it came to me that all this really was an adventure filled with great amount of trust, good judgment and cooperation.
Every decision must weight in risks but also specifics of patient. If you ever looked at kickboxers training or a fight you understand forces and energy that are involved in whole process.
Initial situation
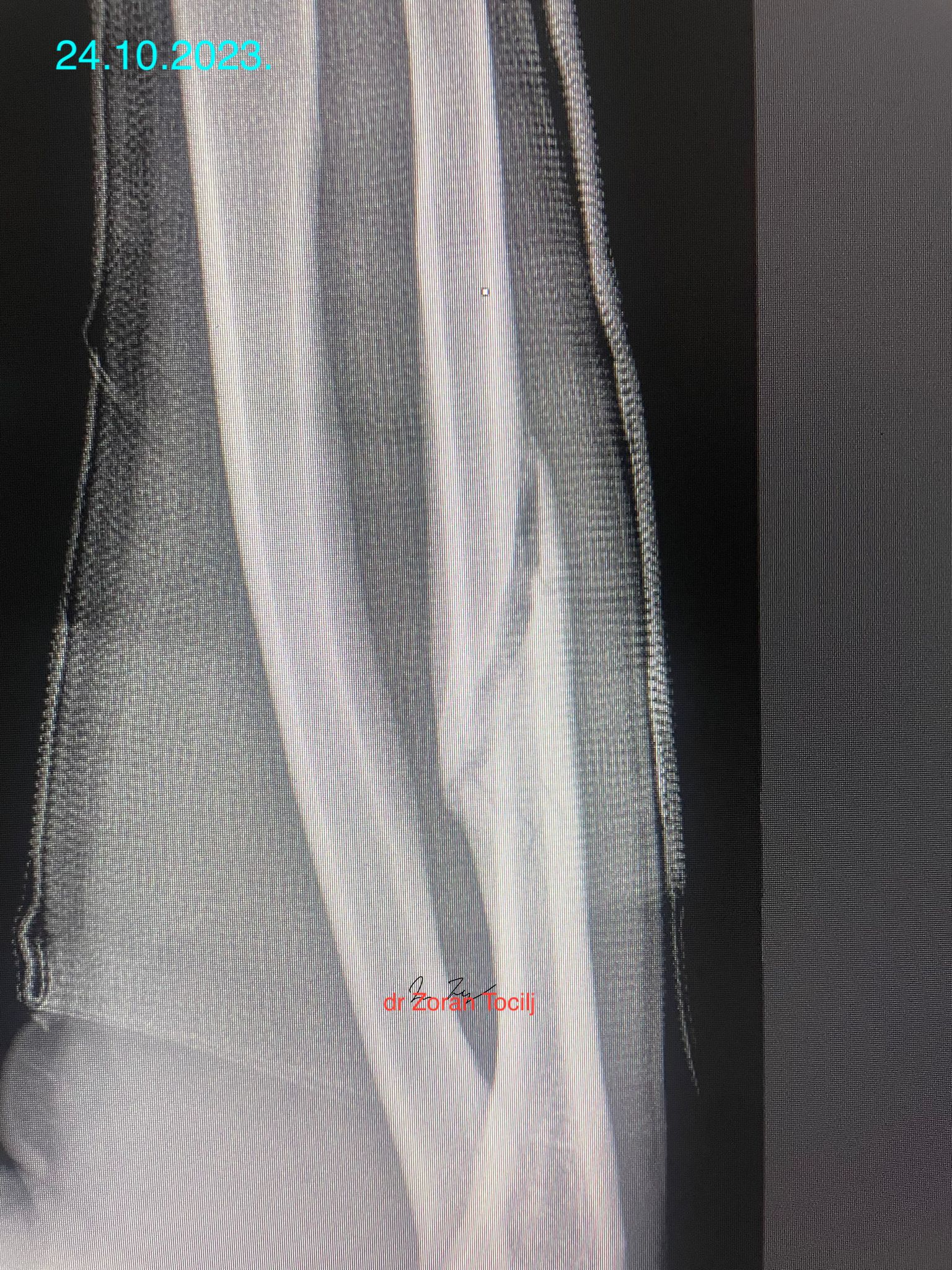
During a kickboxing match a fighter felt sharp pain and snap in his forearm, he continued fighting for whole five rounds!
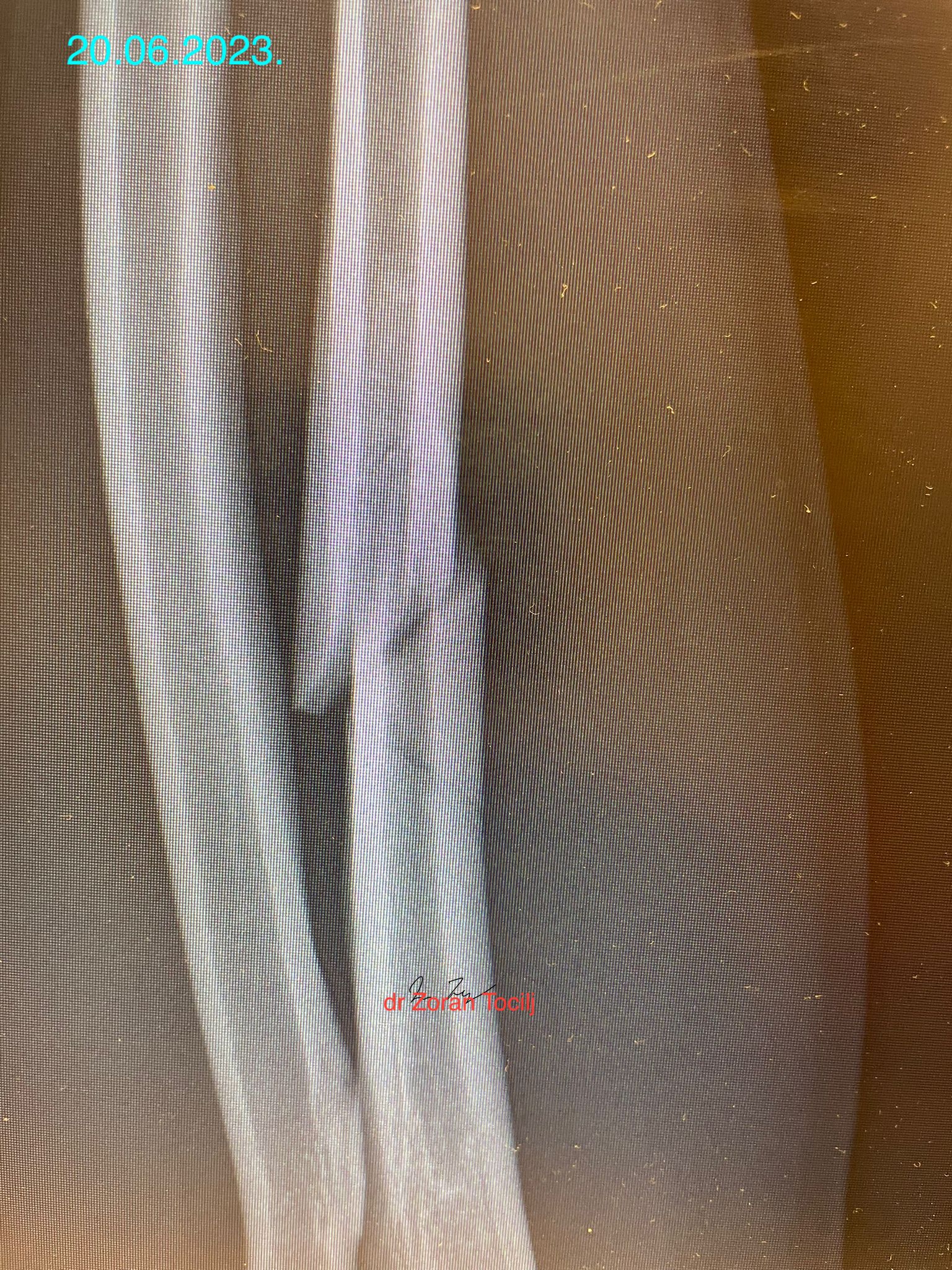
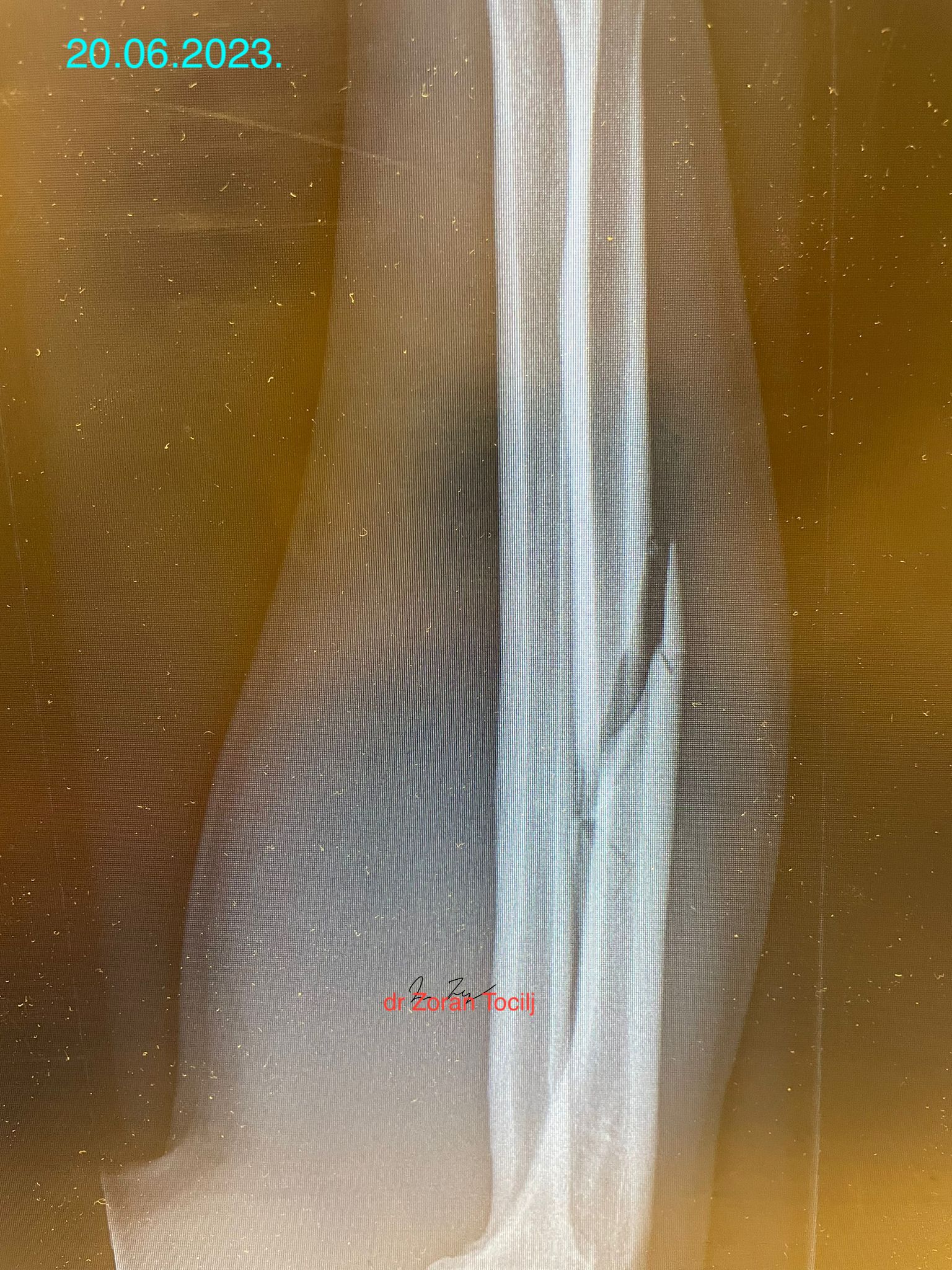
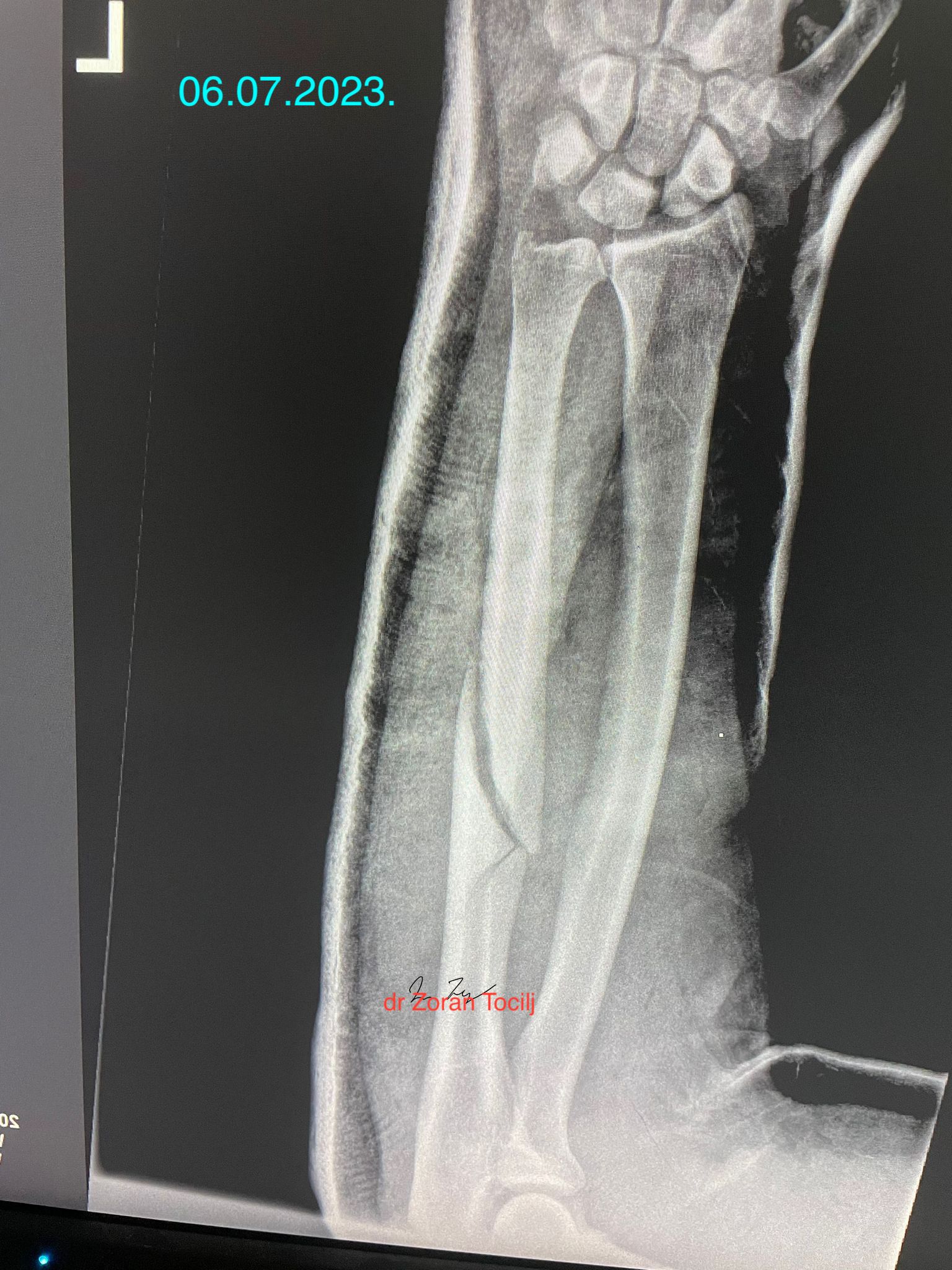
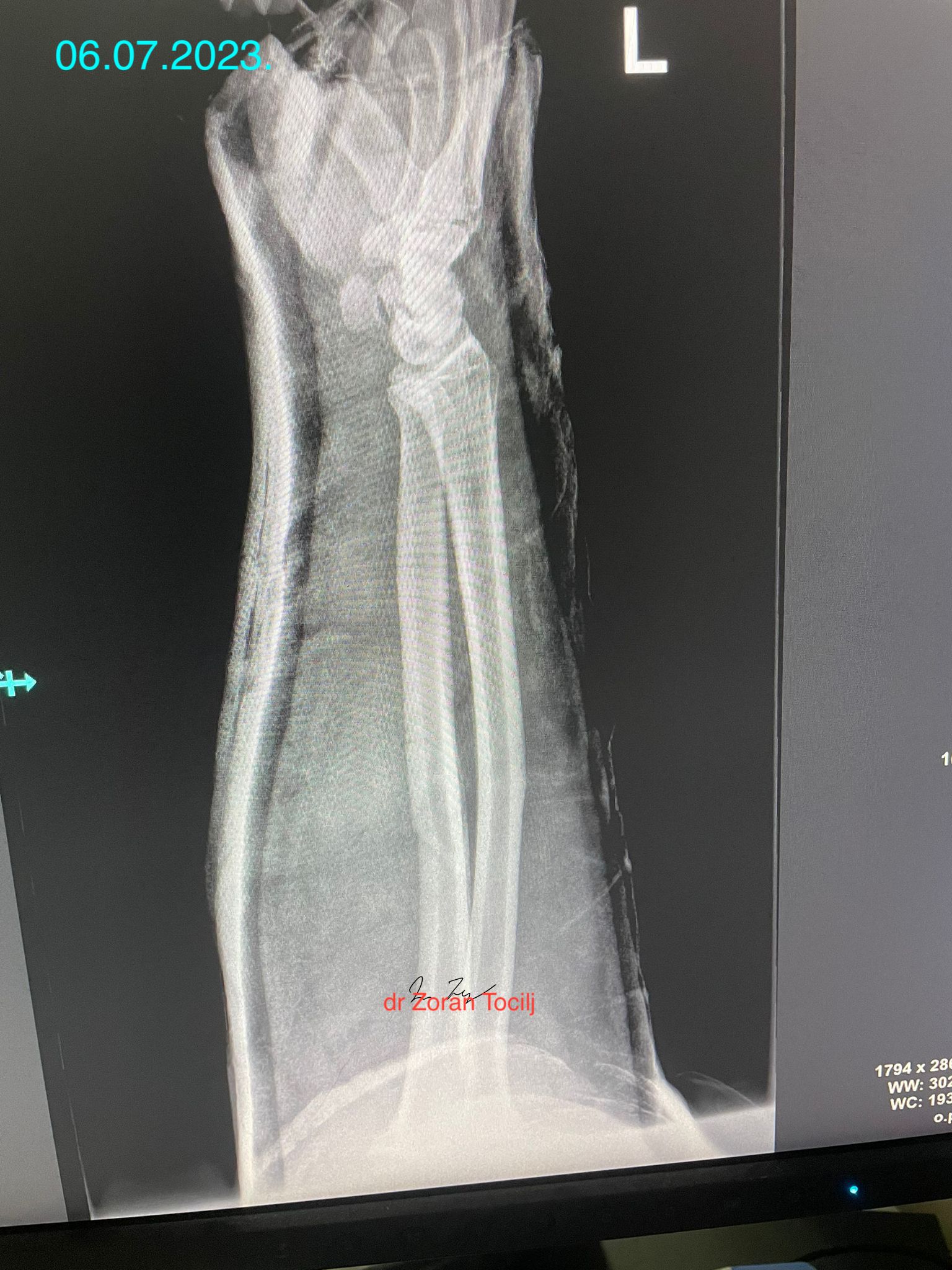
THIS IS THE X-RAY AFTER THE MATCH.X-ray taken right after the fight at ER. Strong forearm held the pieces from completely shattering even though fighter continued the fight with broken forearm!
NOT THE SMARTEST MOVE
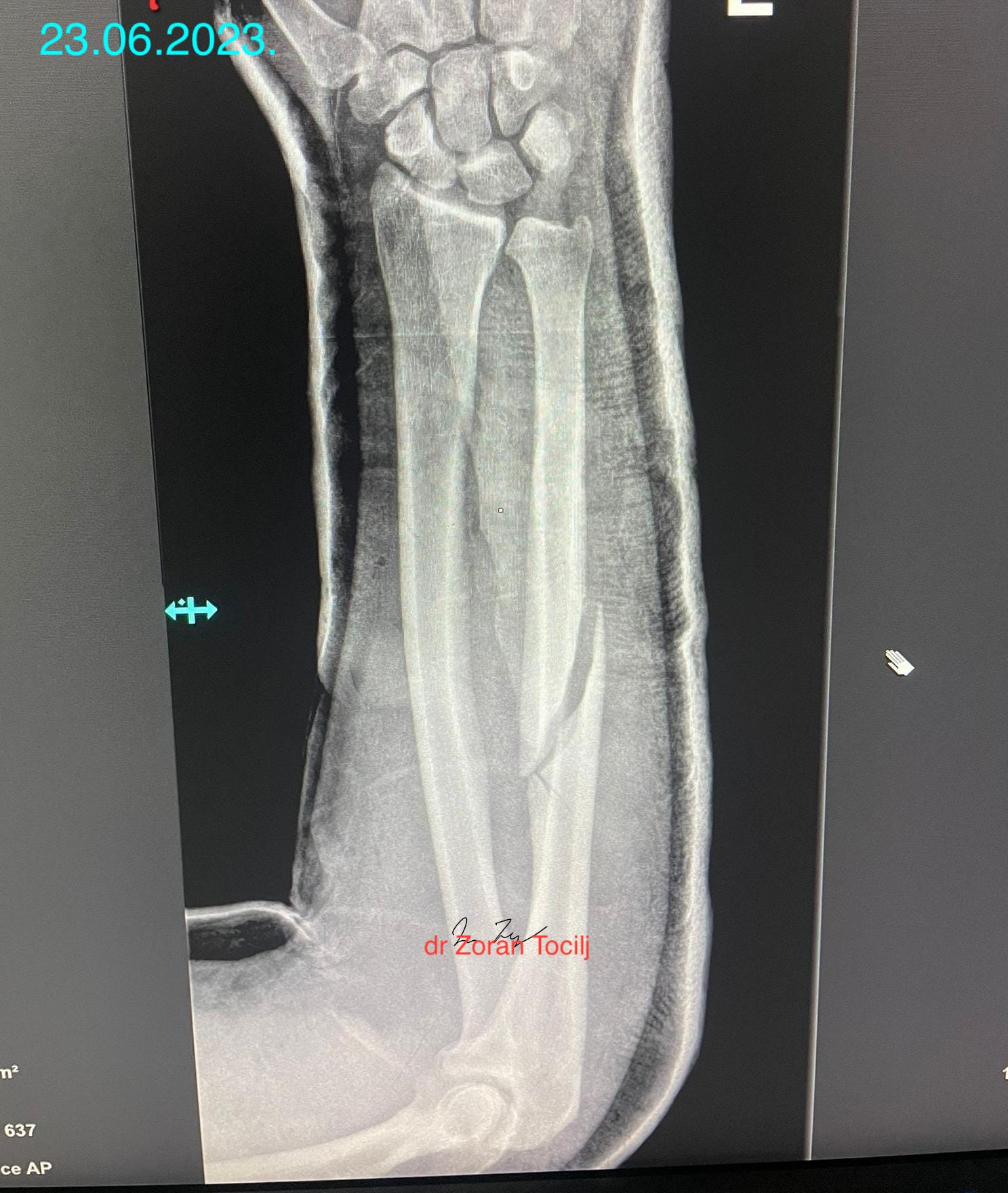
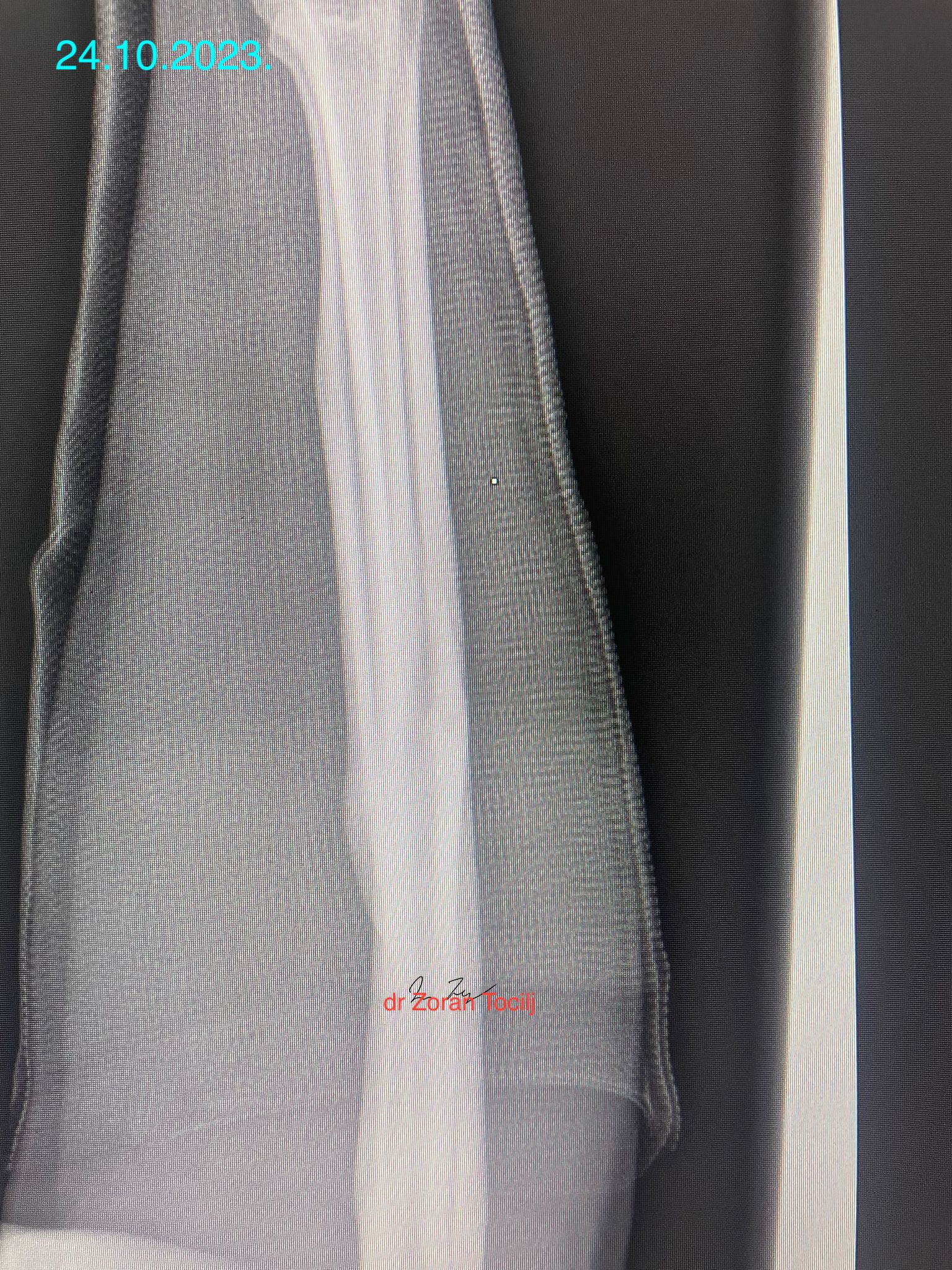
After repositioning, position of bones looked good

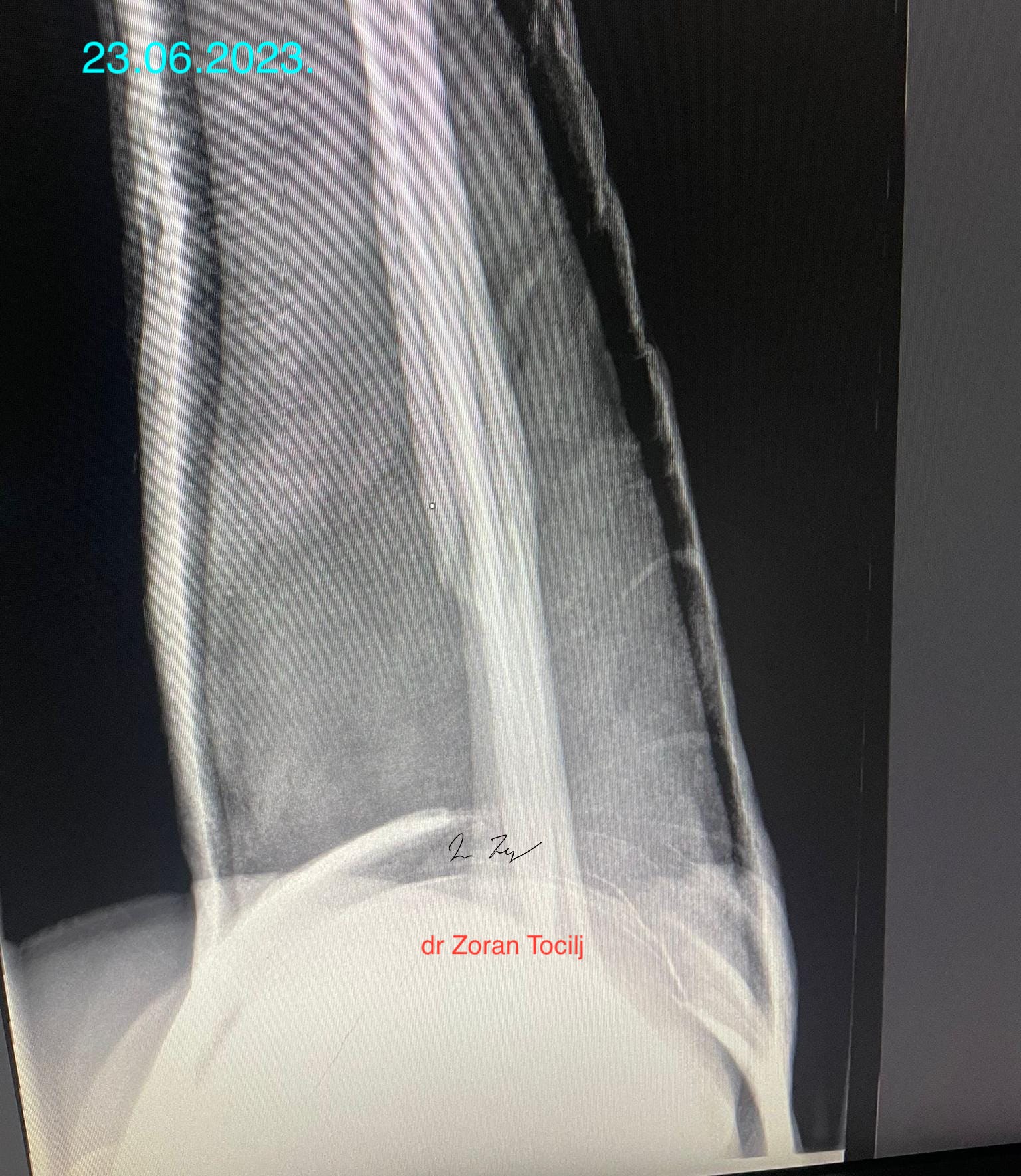
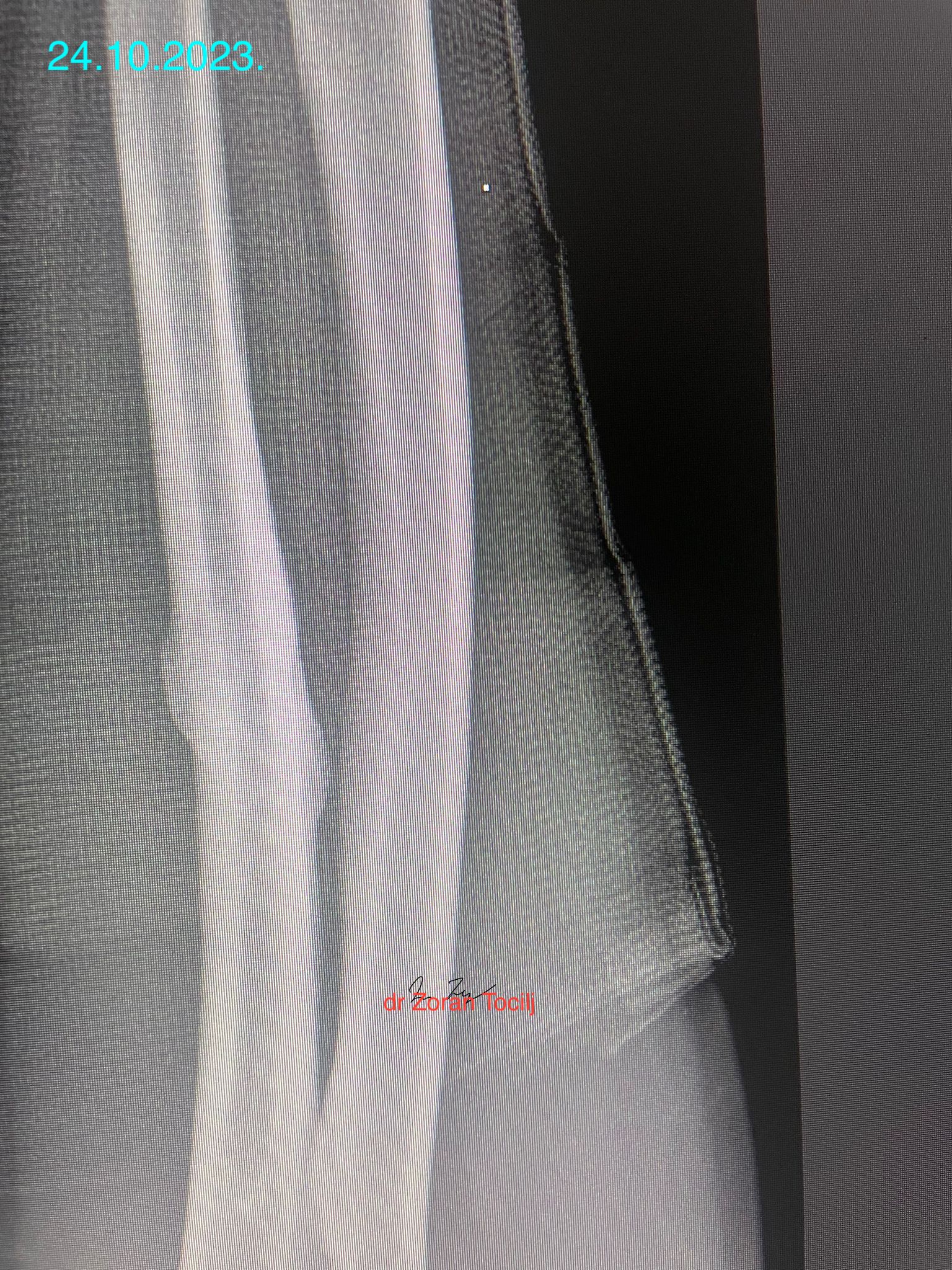
But after control X-ray, things did not look as good:
There was a clearly visible movement of bone fragments. My opinion/guess was that cause of it were contracting muscles of forearm and that any more manipulation would render even great muscle spasm causing even more fragment distancing. So touching anything would do more bad than good, se we hat to go with what we had.
There was a lot of pressure to operate the fracture as the natural healing was not guaranteed (fragments were too apart) and the operation would speed up return to normal activity. I was strongly against, in my experience I had very bad cases in patients whom were involved in explosive hand movements or received kicks in the injured area. I will demonstrate two cases former one is a goalkeeper for one national team and latter is of a MMA fighter.
Goalkeepers receive high energy impacts to the hand from soccer ball and MMA does not need much explanation. Both cases biomechanically can be compared to kickboxing so the logic applies.
Take a note it is not that the operations were a failure, in both cases operations were success but caused additional complications that differed from initial injury!
Operated examples
First Case - goalkeeperGoalkeeper(of one national team) initial ulna fracture was operated and used titanium plate fixation to stabilise, healing was adequate but plating caused biomechanical trauma on distal part of ulna that caused secondary fracture. Second operation removed the first plating as initial fracture healed and used microplate on second fracture to avoid biomechanics stress. Second operation caused new injury and a new fracture but now a bit more proximal in the area od most proximal screw. Third operation put a new plating over second and third fracture. After all this operations forearm was useless for basic tasks like holding things or cutting meat, let alone serious exercise.
(he returned to the pitch after several cycles of therapy that took long time, much longer than needed to heal initial fracture)
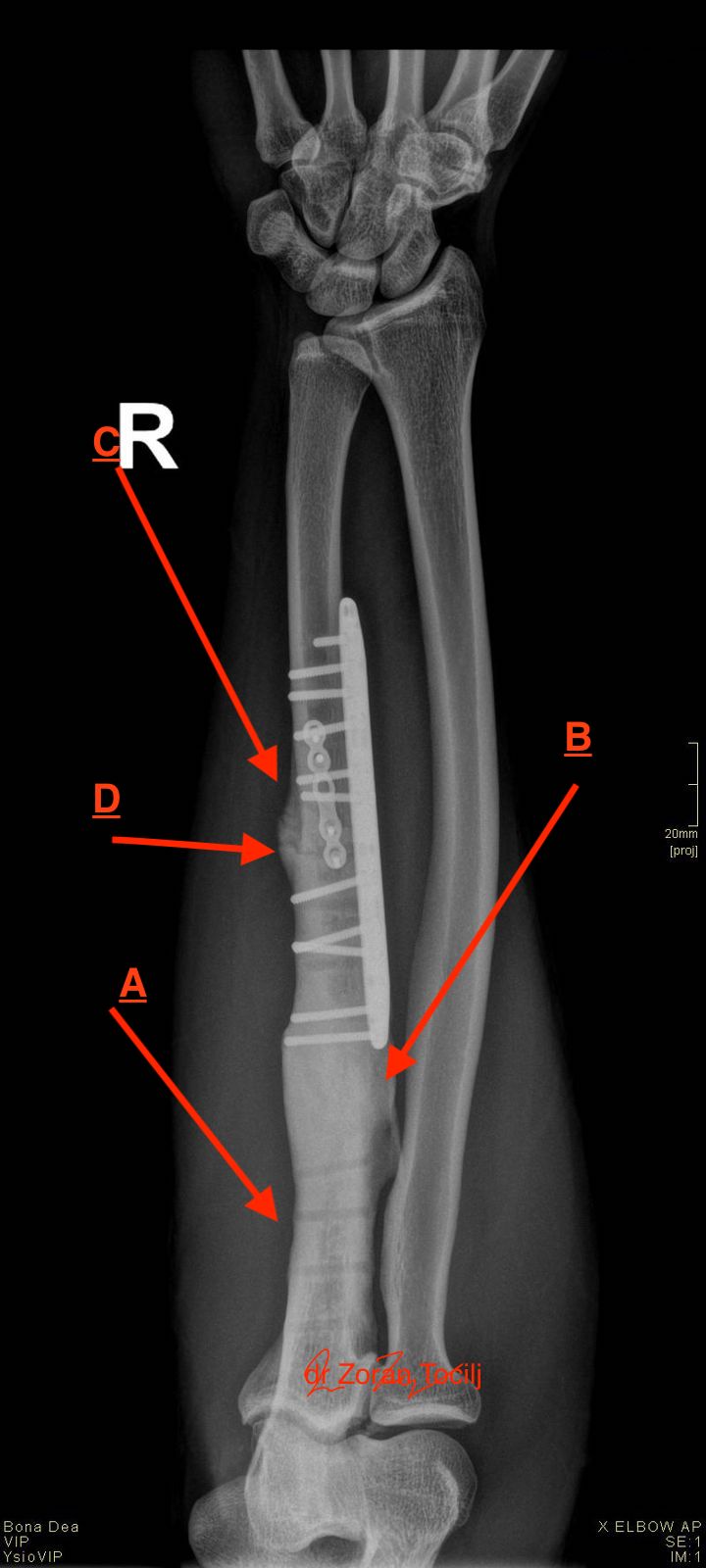
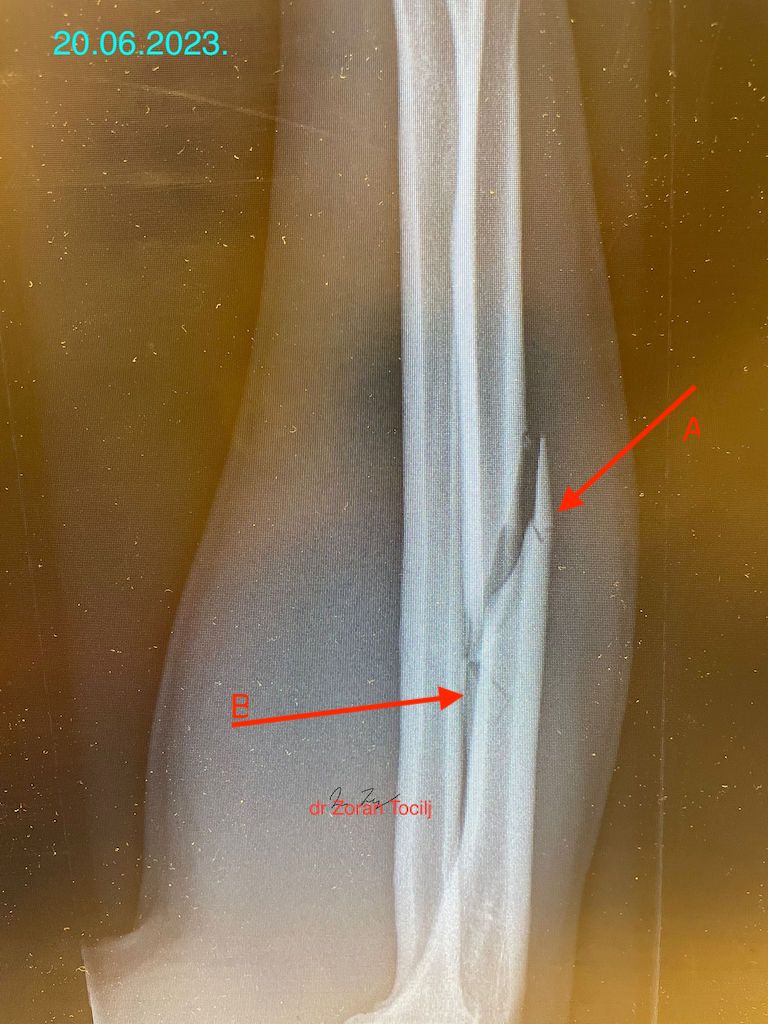
Goalkeeper initial ulna fracture (B) with two additional fractures (C) and (D) after initial fixation
(A) area with screw traces for the first titanic plate fixation for the fracture in area (B)
(B) initial ulna fracture completely healed
(C) secondary partialy fracture and microplante fixation
(D) tertiary unhealed fracture just on the edge of 2nd plate with third plate fixation
Second Case - MMA fighter
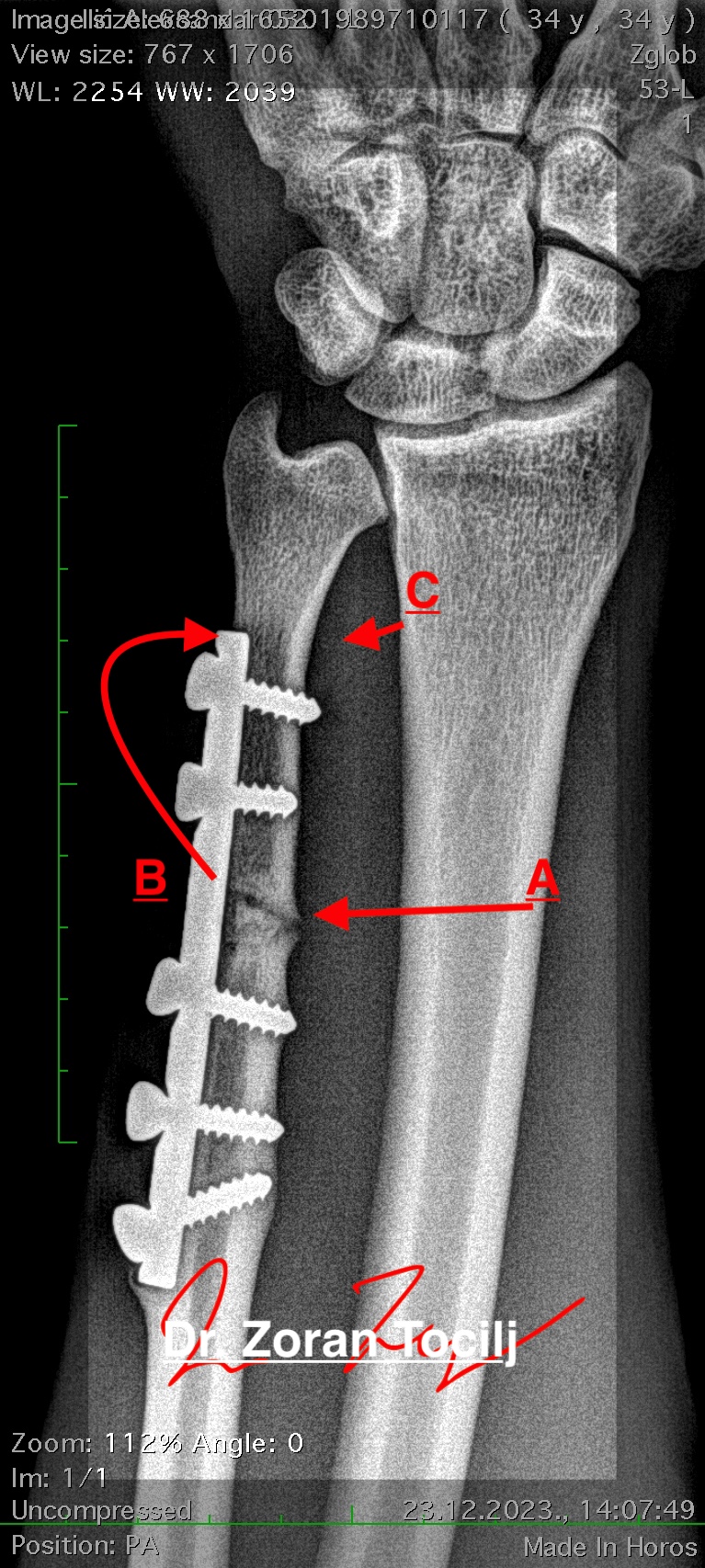
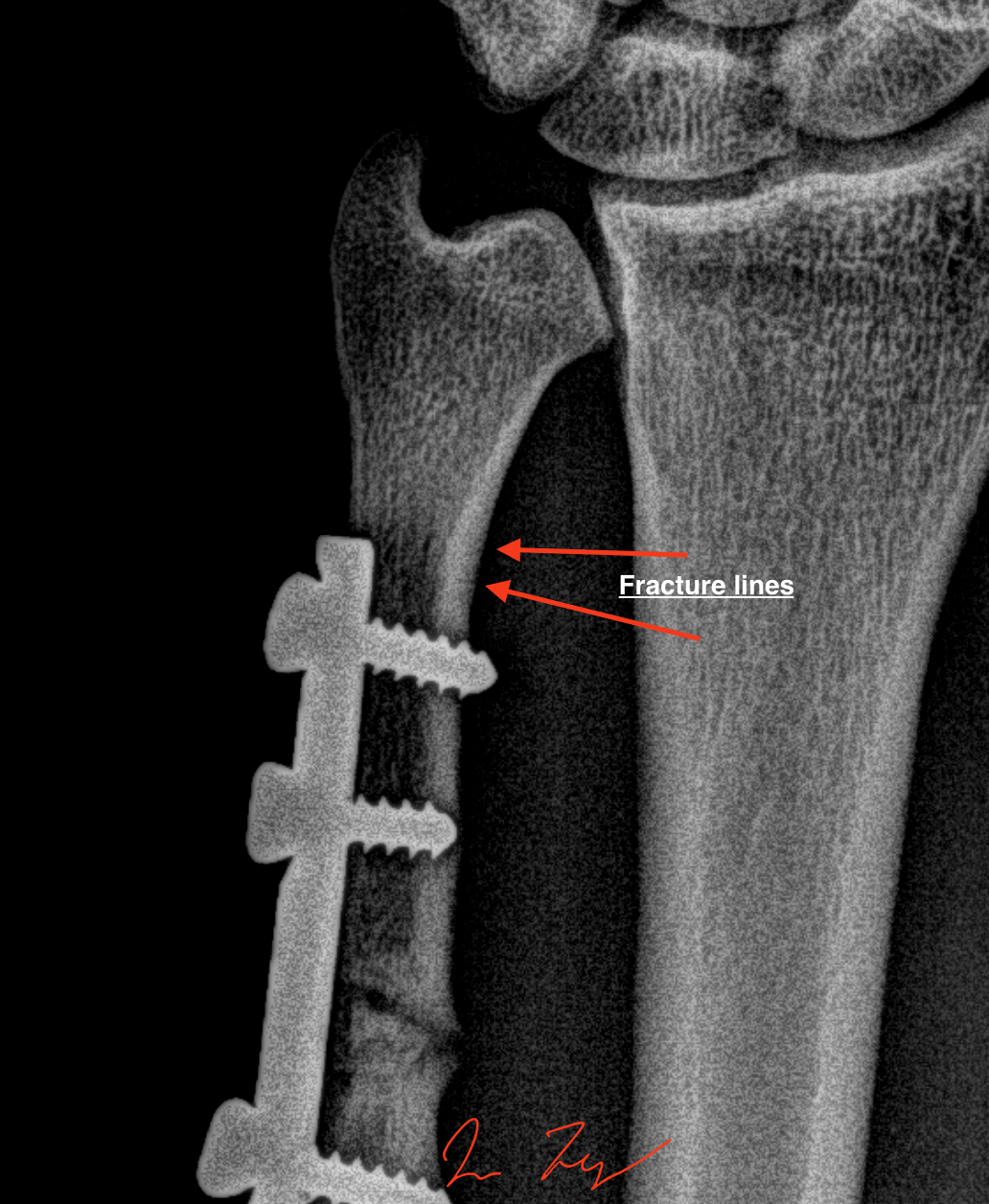
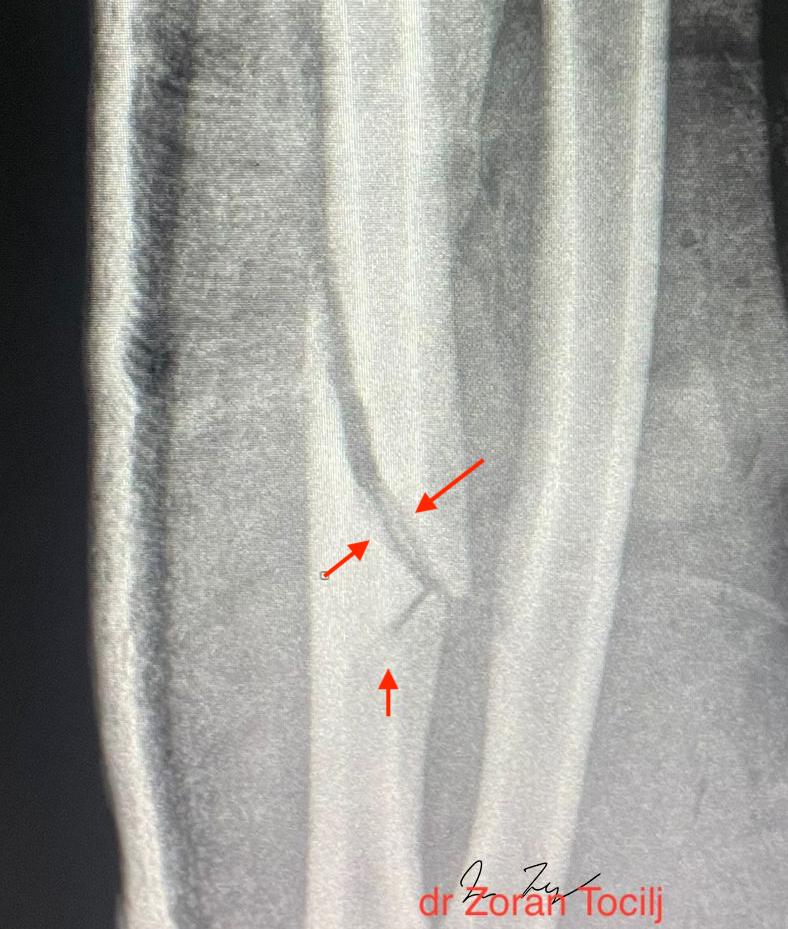
MMA fighter had his ulna fracture operated right after it broke during a fight. After operation, several problems arose, initial fracture has not healed, distal bone shows matrix degradation and two micro fracture lines appeared in distal bone cortex (remember where the goalkeepers arm broke after initial operation!)
(A) initial fracture
(B) bone demineralisation area
(C) fracture lines visible on 2 slide
Healing process
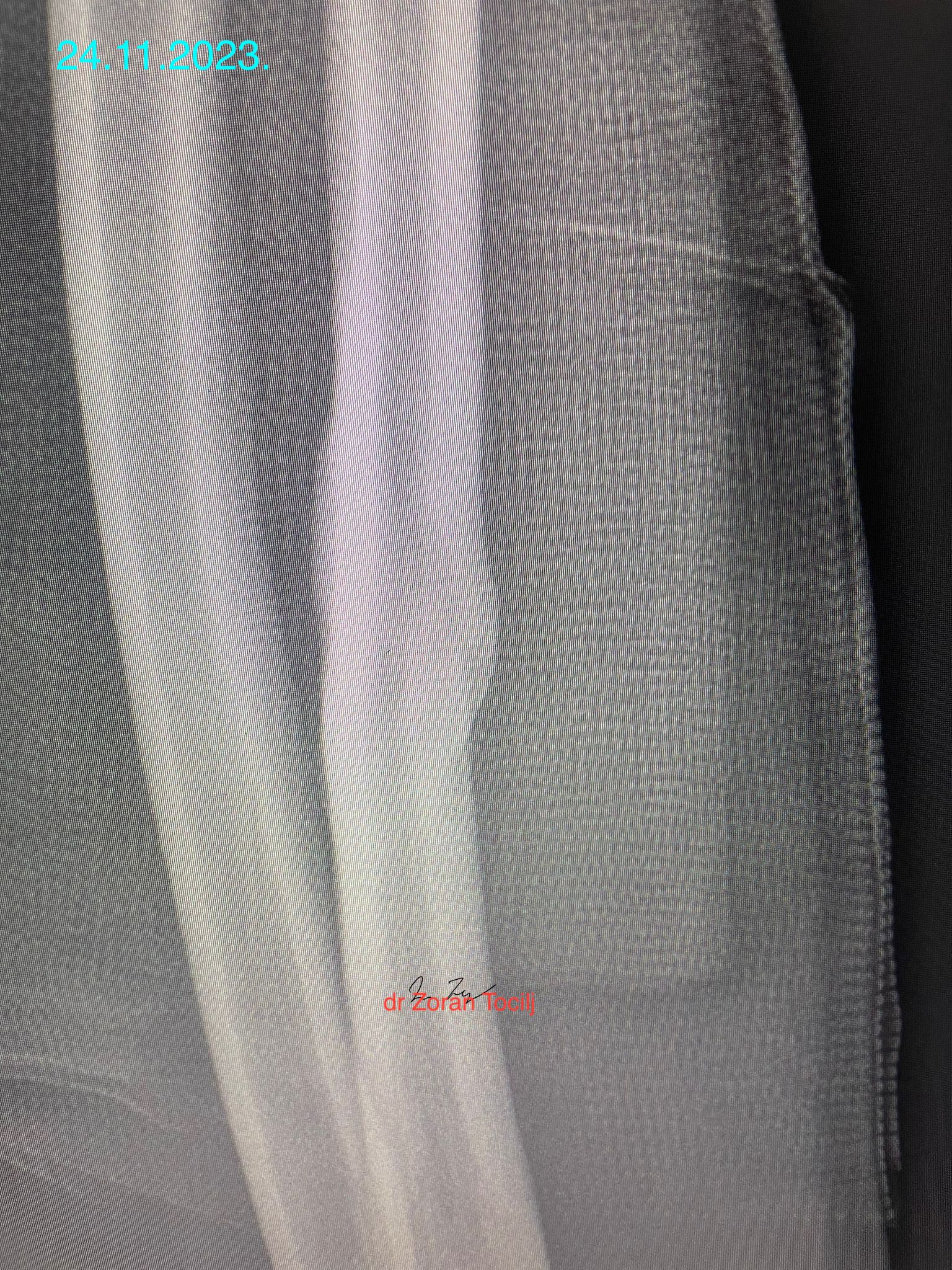
Two weeks... First control X-ray was a key to access if the bones held it place so the regeneration can start. We added a lot of vitamins, especially vitamin D, zinc, omega 3, calcium, amino acids but within first two-three week I expected bone demineralisation and fibrosus hematoma formation. The proof would be stability of bone fragments and no change on X-ray.
The fact that bones did not move suggested some kind of soft fibrous tissue forming (not calus yet). Bones look a bit softer on edges that is a good sign.
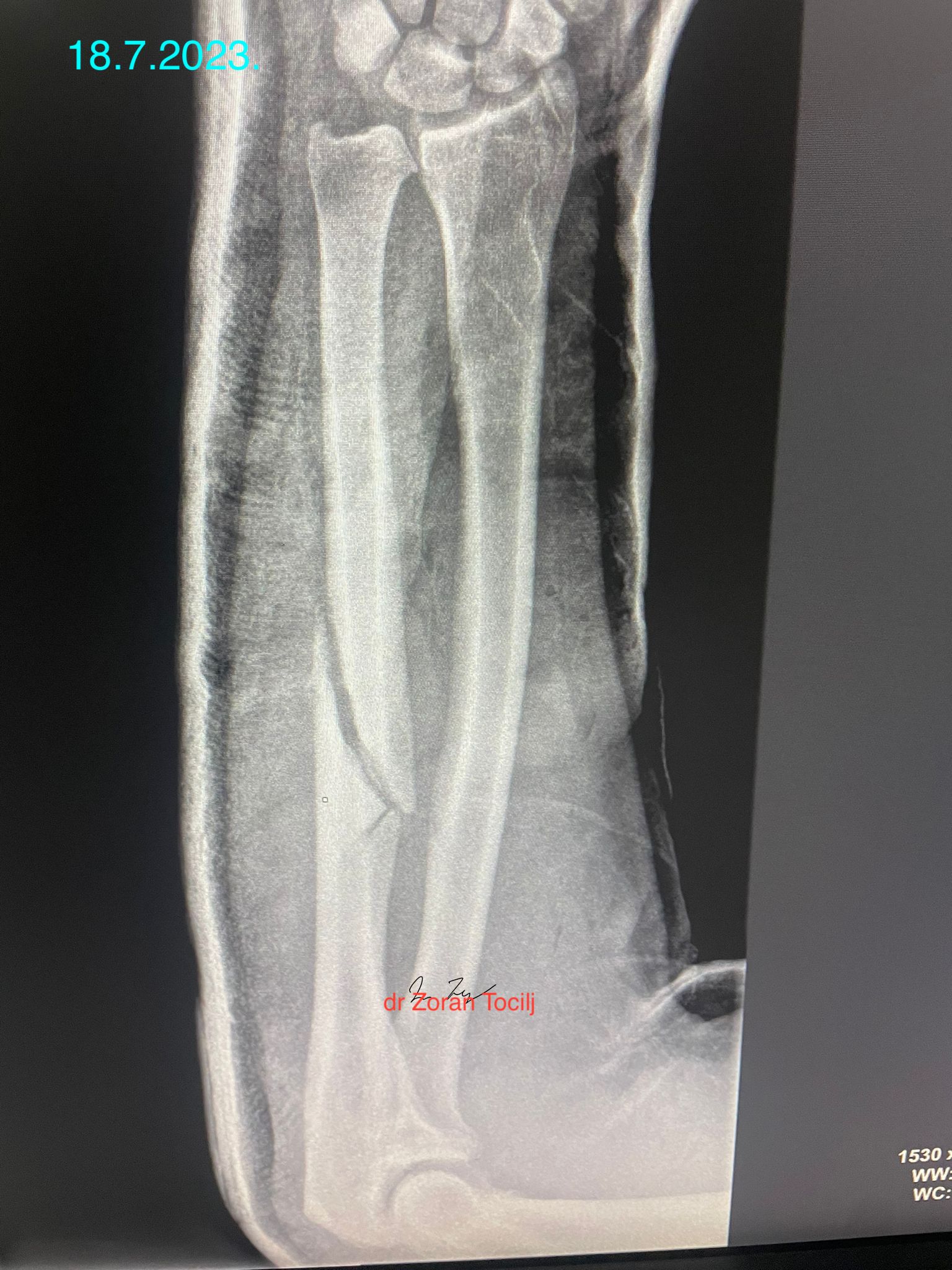
Four weeks... Control X-ray should show slight changes
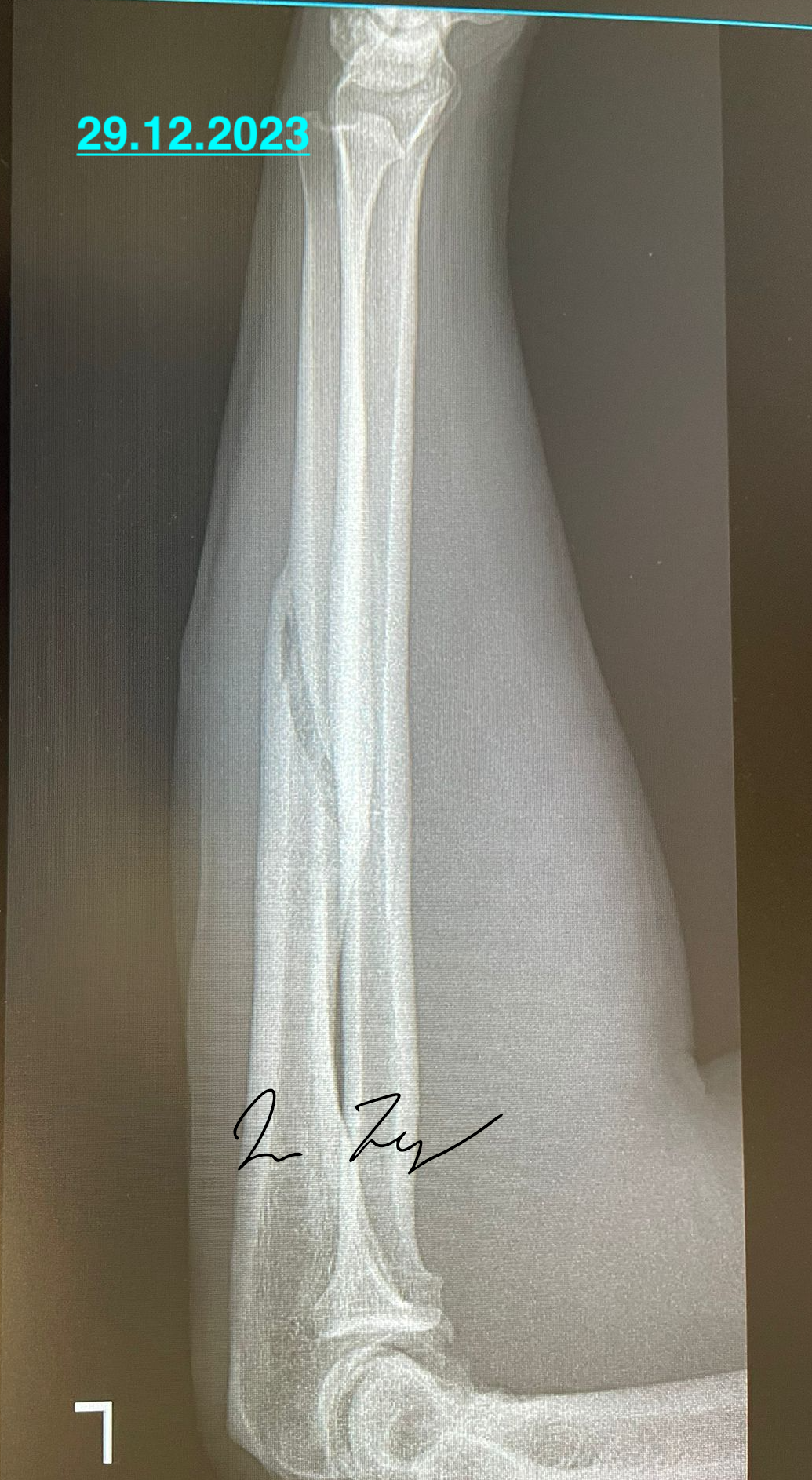
There was definite change in X-ray, slight calus/interosseal calcification, but without definite contact. Calus can not be visible through old plaster (and in Split believe or not there was no option to change it for a plastic one).
Nine weeks... Control X-ray should show changes, bones connecting in closes part. We made a small modification to the plaster, a hole in non supportive part so fracture can be accessed by direct injection of prolotherapy in fracture.
It is important to note that vitamin and mineral support was continuous and hand was active as much as plaster allowed it to be. Opposite hand was normal used for one arm training (thanks to a excellent gym trainer for finding proper solutions Ivan Bancek Vukas)
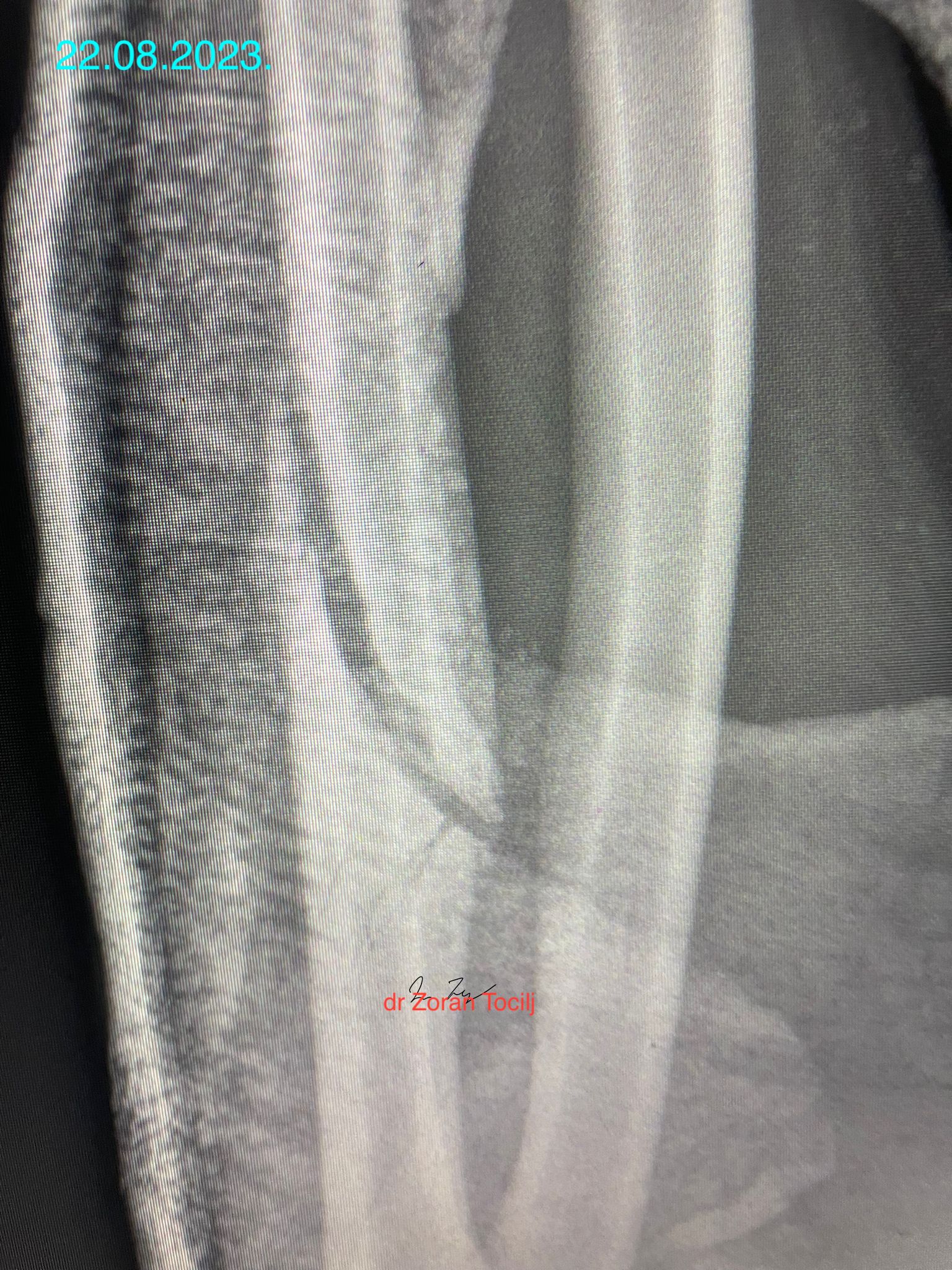
Eighteen weeks later...
In the meantime local prolotherapy was continued to a point where patient reaction suggested that bone healing progressed to complete fracture stability. Following that, plaster was changed with a plastic one and new X-ray was made. Hand was almost fully mobile in new plaster so more exercises could be included (by ex medal winning weightlifter and excellent trainer Eni Music)
Clear healing progression fully visible.
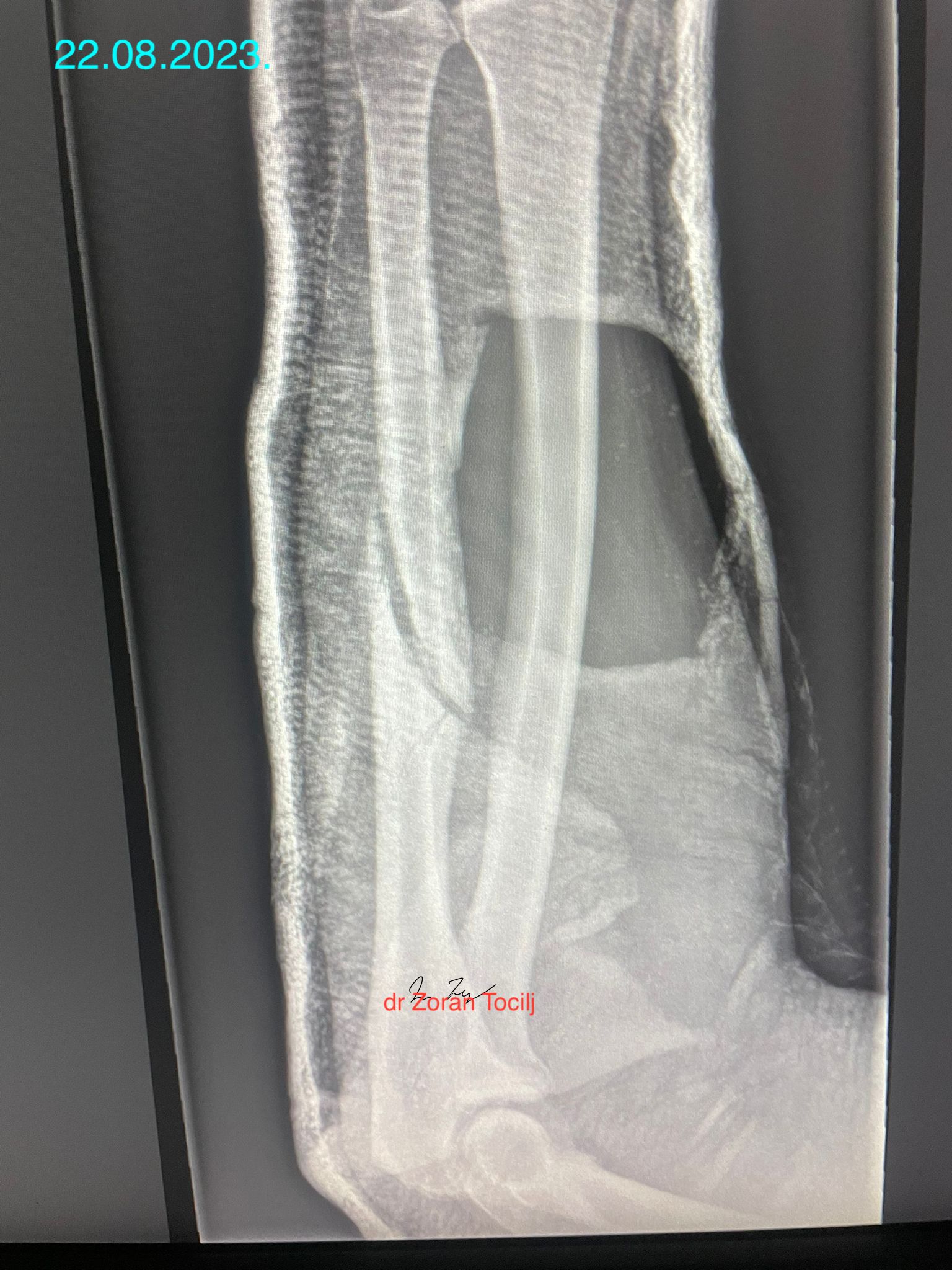
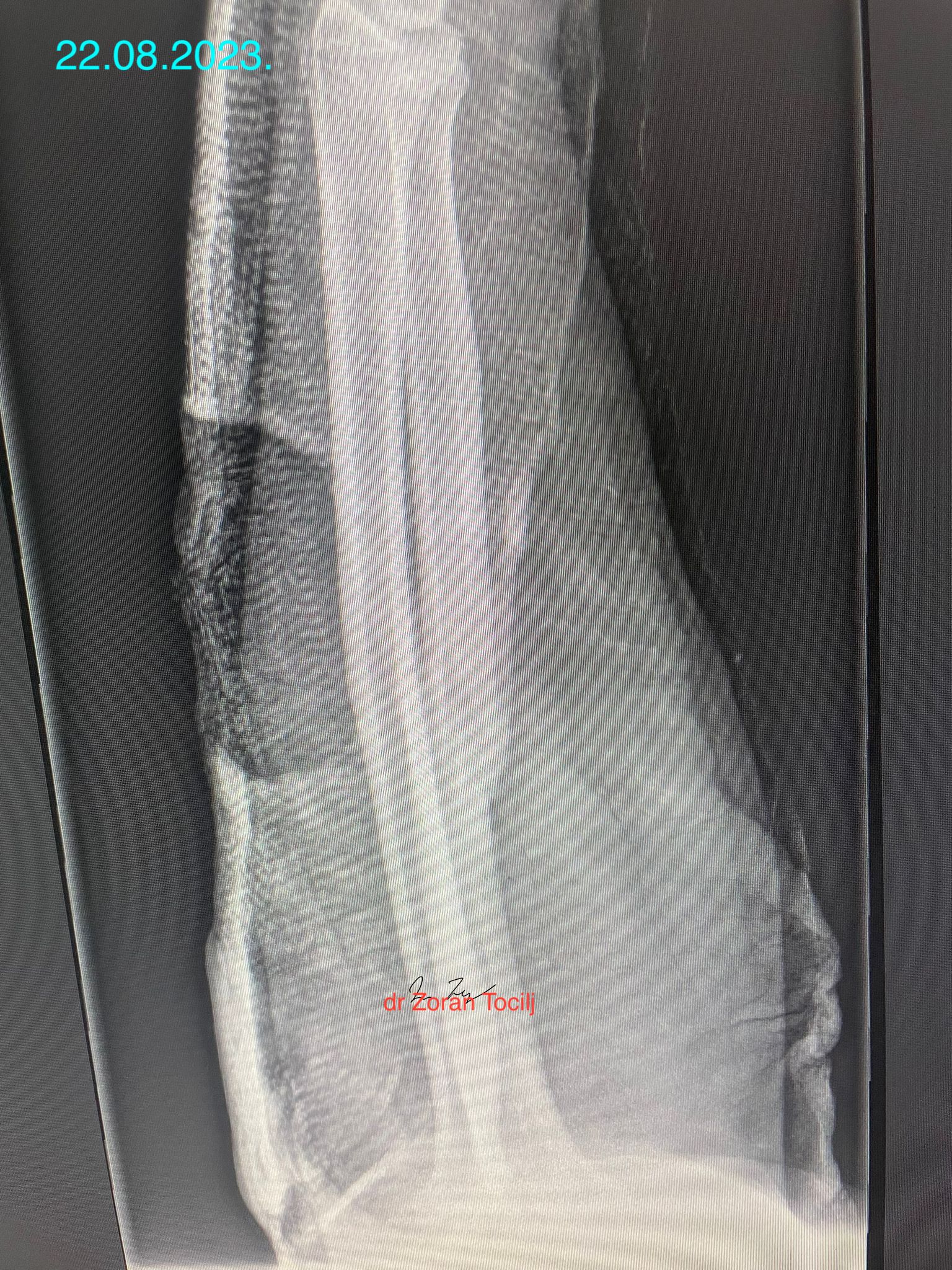
Twenty-two weeks later...
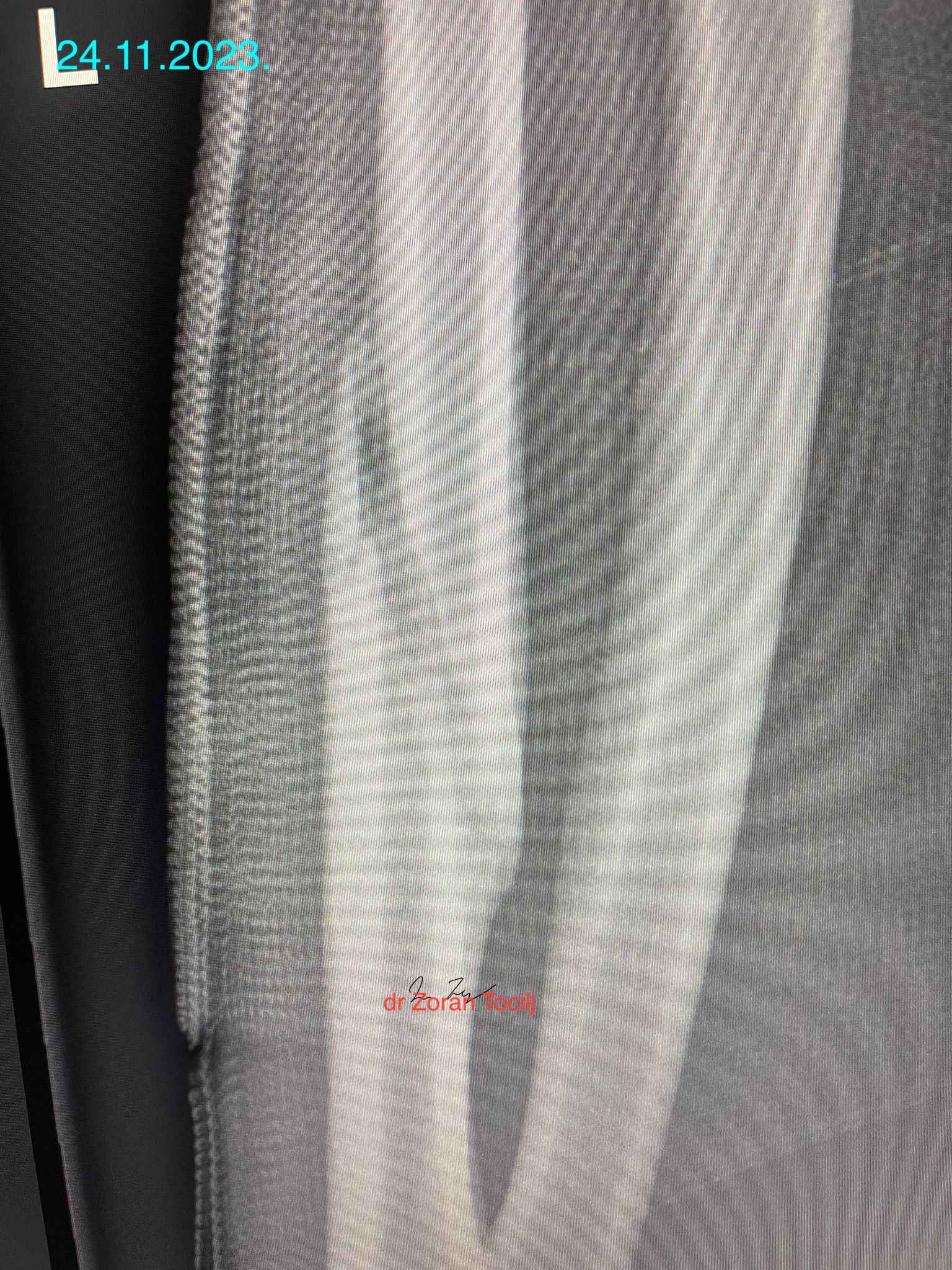
At this point it was decided to remove the plaster that served more as fashion item than any useful kind of stabilisation or protection.
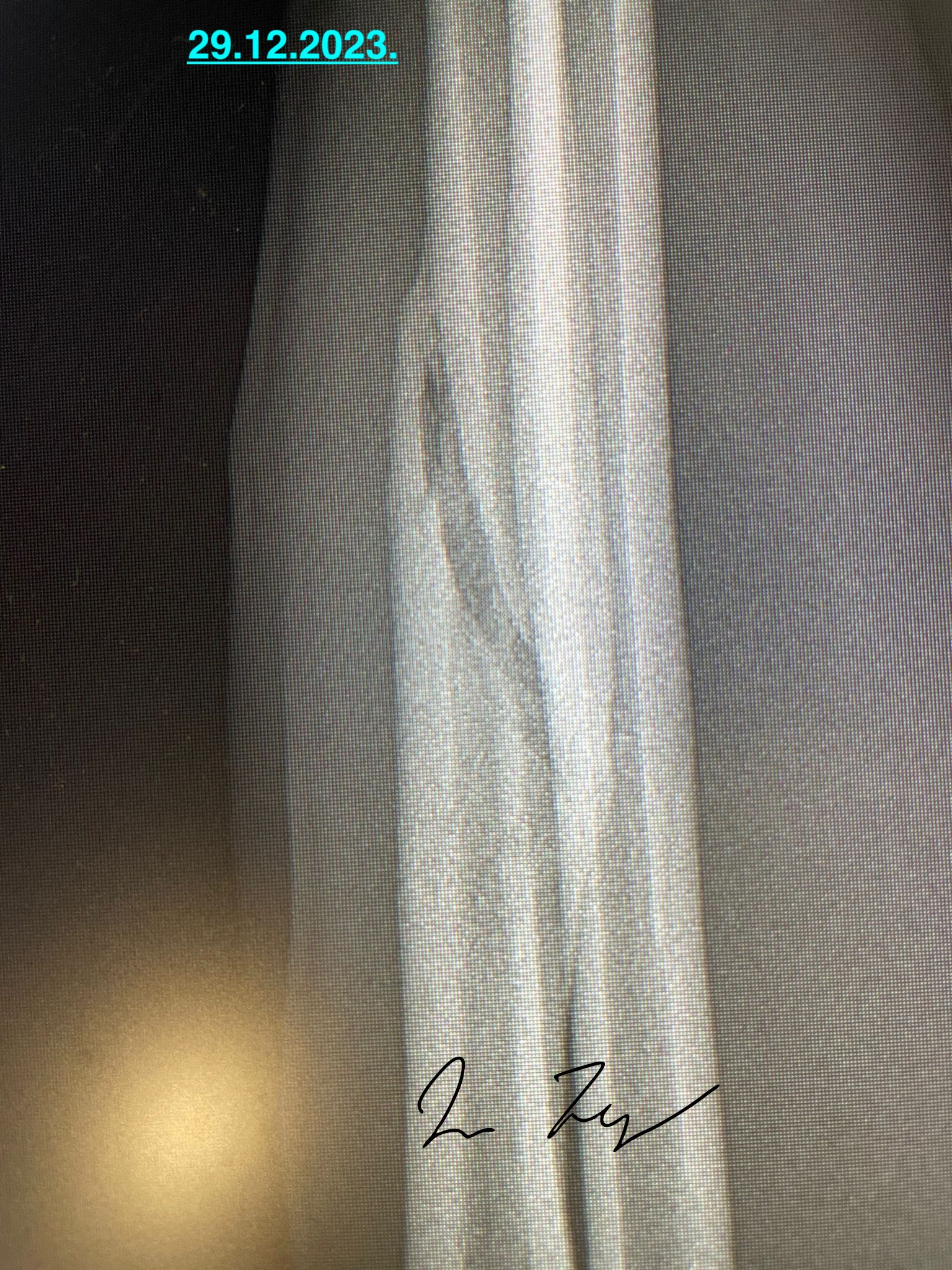
At this point fracture is stable enough to consider it a completely healed and to return fighter progressively to full activity. Additional bisphosphanates were applied directly to injured area to stabilise calcium matrix of the bone.
It passed 192 days from initial fracture to full healing. During that time all guidelines for vitamin intake were followed(although it looks insignificant, proper intake is essential for healing of bones) and prolotherapy were applied with additional bisphosphanates at very end of therapy. All the time maximum movement/exercise, that was possible, was advised.
All therapies were in full accordance with WADA antidoping guidelines 2023.